
Tendon Pain and Exercise: Avoiding the Boom–Bust Cycle
Most injuries don’t come out of nowhere—they’re the result of a mismatch between what your body can handle and what you ask of it. This “boom-bust” cycle is common in tendon and tissue injuries, where periods of high motivation and overload are followed by pain, rest, and frustration. Understanding how to build and respect tissue capacity is the key to staying active, consistent, and injury-free.

New Year, New Foot Pain? Understanding Overuse Injuries

What is Shockwave Therapy?

Diabetes and Foot Health: How to Prevent Complications Before They Start
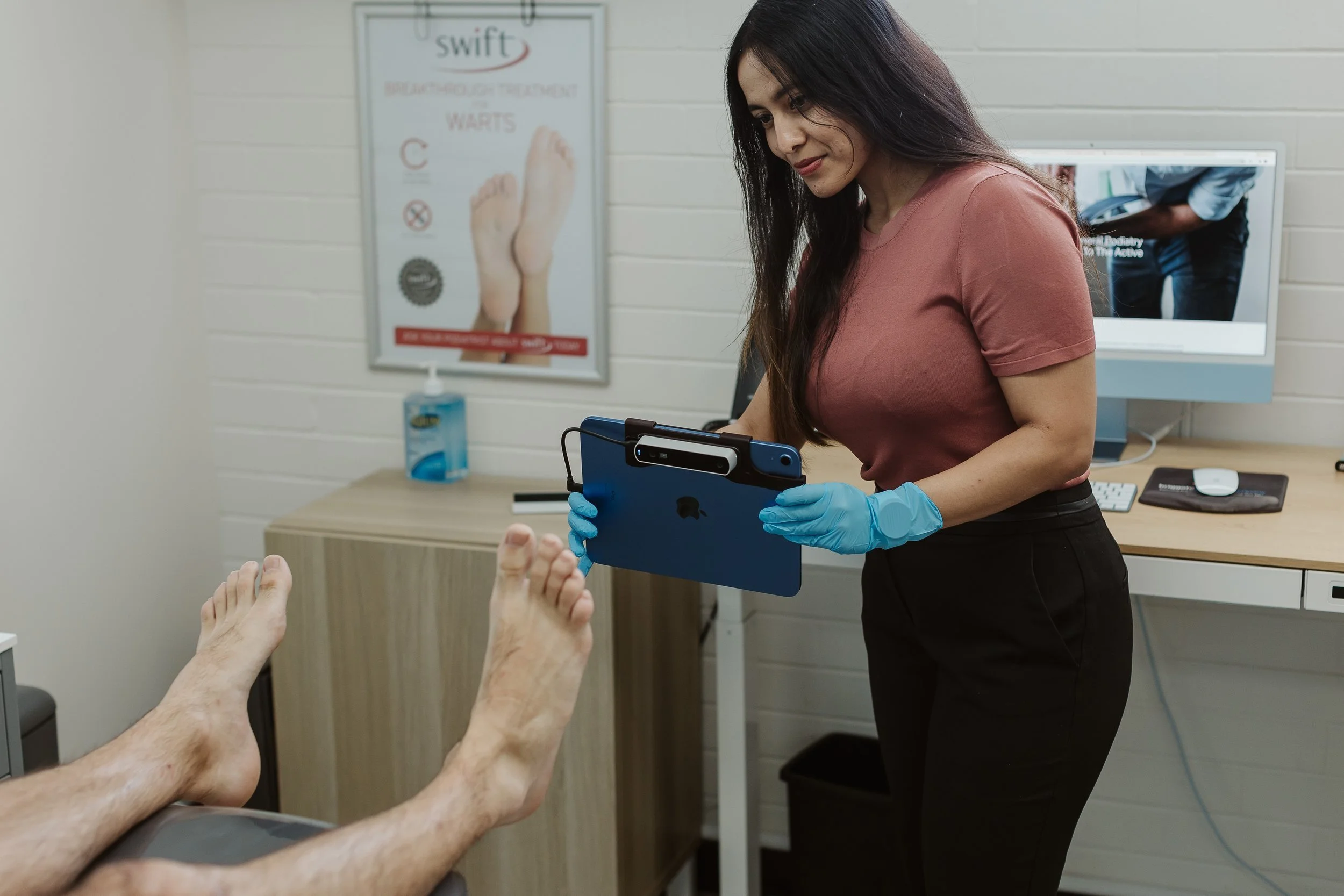
Our podiatrist - Mathew Millar - performing a Doppler Ultrasound test to assess a pateint’s blood flow to her feet.

Top 5 Tips for Preventing Common Running Injuries

Finding Your Perfect Fit: A Podiatrist's Guide to Running Shoes
Finding Your Perfect Fit: A Podiatrist's Guide to Running Shoes
As podiatrists, we see a wide range of foot-related issues stemming from ill-fitting footwear. And when it comes to running, a proper shoe fit is absolutely crucial for preventing injuries and maximizing performance. Whether you're a seasoned marathoner or just starting your running journey, understanding how to select the right shoe is paramount.

Chronic Ankle Instability: When a Simple Sprain Becomes a Long Term Problem

Understanding Bunions: What You Need to Know and Why Treatment Matters

Ankle Sprains 101: A Sports Podiatrist's Guide

Metatarsal Stress Fracture? Is Your Foot Trying to Tell You Something?

Suffering From Burning or Numb Toes? We Can Help!
Painful Morton’s Neuroma
How to Treat and Prevent Shin Splints

What Is The Significance Of Gait Analysis In Achieving Optimal Movement And Overall Well-Being?
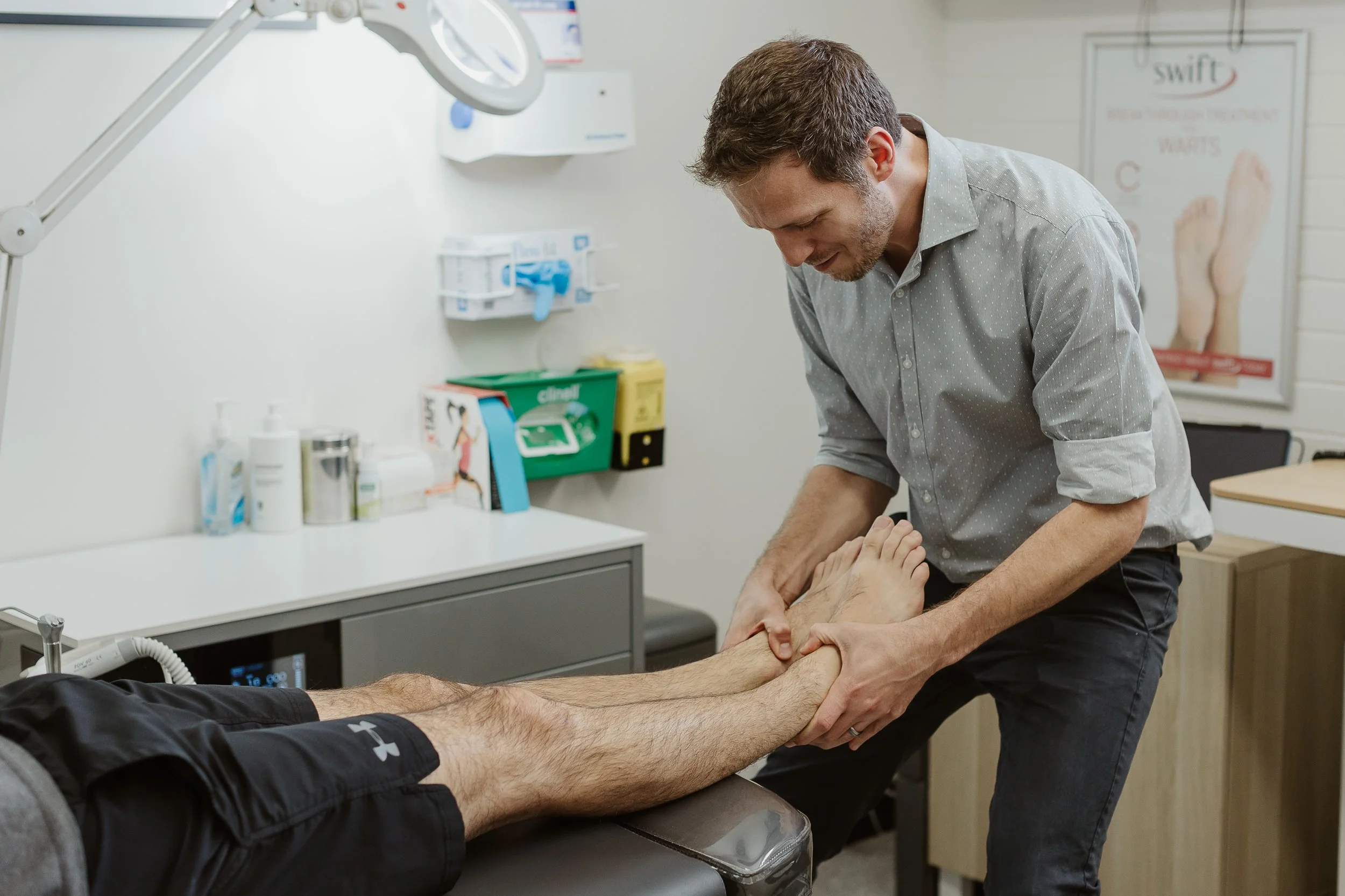
During a biomechanical assessment, podiatrists carefully examine the way a patient walks, runs and moves to identify any issues with their foot and ankle mechanics. By pinpointing these issues, podiatrists can create a personalised treatment plan that often addresses symptoms' causes to help alleviate pain, improve function, and prevent future injuries.
Understanding Achilles Tendinopathy: Midportion vs. Insertional

Say Goodbye to Warts Using SWIFT Microwave Therapy

Why Would You Choose Prolotherapy Over A Cortisone Injection?

Are Flat Feet Bad?

Why I Should See My Podiatrist For a Biomechanical Assessment?

How to Treat Ingrown Toenails Without Surgery
Do you want to know how your podiatrist can treat ingrown toenais without surgery?

